First endobronchial ultrasound procedures in PH
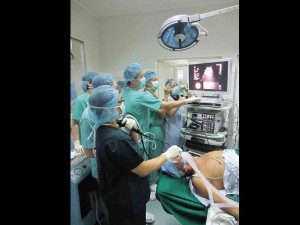
DALUPANG (left, holding an instrument) performs the country’s first Ebus-TBNA procedure on a patient suspected to have lung cancer. He also performed the first Ebus-GS in the country on another patient with peripheral pulmonary nodule.
To recommend the best treatment for one’s lung cancer, it is very important for the doctor to know how far the cancer has progressed.
This is because an accurate staging of the lung cancer could spare the patient from going through surgery, especially if the cancer could still be treated by other less invasive means such chemotherapy or radiation.
If surgery is the best option, an accurate staging of the lung cancer could reduce the amount of tissues that will be removed during surgery, thus reducing the likelihood of complications and helping the patient recover faster.
Last week, the Center for Respiratory Medicine Interventional Pulmonology of the University of Santo Tomas Hospital announced that it just performed the first four successful endobronchial ultrasound (Ebus) procedures in the Philippines.
Ultrasound technology
The Ebus is a relatively new procedure that provides real-time imaging, enabling pulmonologists and thoracic surgeons to see through the walls of patients’ airways and into chest and lung tissue. This is important in order to obtain biopsies of tumors, masses and lymph nodes that aid in diagnosis and treatment.
The procedure was performed by a team of surgeons led by Dr. Julius Dalupang, regarded as the first Filipino interventional pulmonologist and pioneer in advanced diagnostic and therapeutic minimally invasive pulmonary procedures in the country.
Dalupang’s team is composed of interventional pulmonologist Dr. Christine Chavez, anesthesiologist Dr. Ethel Guerrero, as well as Dr. Irene Vergara and Dr. Mark Flores.
View and evaluate
“Ebus allows a doctor to perform a technique known as transbronchial needle aspiration (TBNA) to obtain tissue or fluid samples from the lungs and surrounding lymph nodes without resorting to conventional surgery. The samples could be used for diagnosing and staging lung cancer, detecting infections and identifying inflammatory diseases that affect the lungs, such as sarcoidosis or other cancers like lymphoma,” explained Dalupang, who trained at the University of California in San Diego, and has been for the last 13 years performing other interventional pulmonary procedures such as endobronchial electrocautery, argon plasma coagulation and Nd:YAG laser resection of malignant and benign airway lesions, and airway stenting.
In a number of countries, the Ebus-TBNA has become the initial procedure of choice in staging lung cancer in patients as this makes biopsies safer and more accurate than conventional “blind” TBNA. It also provides a less invasive, less costly alternative to mediastinoscopy (a surgical procedure that opens up and examines the inside of the upper chest between and in front of the lungs).
“Before the introduction of this procedure here in UST Hospital, the lymph nodes could only be biopsied through more invasive or open surgical procedures such as mediastinoscopy and open thoracotomy. Moreover, by employing Ebus, a doctor could now perform biopsy to very small pulmonary nodules in the lung through a guide sheath,(a procedure known as Ebus-GS),” said Dalupang.
Difficult to biopsy
He noted that in the past, these small nodules are technically difficult to biopsy without running the risks of complications.
“With Ebus guidance, a guide sheath can be safely positioned in the tumors,” said Dalupang, who added that the UST Hospital Interventional Pulmonology team has also performed the country’s first two cases of Ebus-GS on patients with peripheral pulmonary mass.
Meanwhile, the UST Center for Respiratory Medicine continues to spearhead bronchoscopy education in the country when it recently held its 4th Bronchoscopy Workshop, entitled “Bronchoscopy Masters: From Fundamentals to the Future,” at the UST Benavides Cancer Institute last May 3 to 4.
The workshop invited guest faculty, professors Dr. Shinji Sasada and Dr. Takehiro Izumo of Tokyo, Japan’s National Cancer Center, the institution where the flexible bronchoscope was invented.
The two experts facilitated the training on endobronchial ultrasound to 36 pulmonary fellows-in-training and 14 pulmonary consultants from all over the country.
Incidentally, this is also the first workshop on endobronchial ultrasound held in the country.














